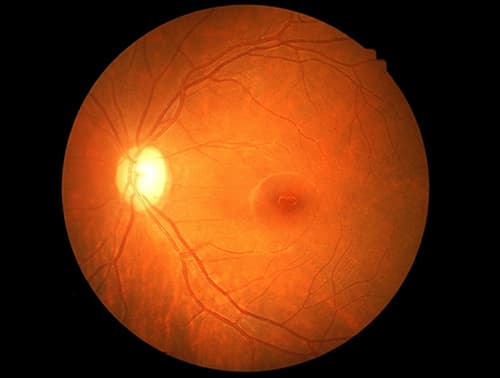
Changes in the retina between healthy individuals and this group could identify patients who haven’t advanced to dementia, while additional changes as Alzheimer’s worsens could track its progression. This is the first quantitative analysis of the retinas of MCI patients, which is an important population because these people are experiencing the earliest symptomatic stages of Alzheimer’s disease, says Yosef Koronyo, a neuroscientist also at Cedars Sinai Medical Center, who developed many of the techniques used in the current research. Donors ranged from healthy individuals to those with mild cognitive impairment (MCI) to Alzheimer’s disease patients with dementia. In 39 cases, the researchers assessed the retina and brain of the same subject, making a direct comparison possible. 
They also looked at the relationship between retinal damage and cognitive decline. The post-mortem study, which looked at retinal and brain tissue samples from 86 human donors, examined potential biomarkers in the retina and linked them to known indicators of Alzheimer’s disease like amyloid plaques (between neurons) and neurofibrillary tangles (inside neurons). “We’re really moving in recent years from a clinical diagnosis, based on symptoms, to a biological definition, based on biomarkers,” or measurable signals such as fasting blood sugar levels for diabetes. Lerner, who was not involved in the research, calls such efforts to develop diagnostic tests “a sea change” in how the scientific community regards Alzheimer’s disease. In fact, the amount of this misfolded protein in a patient’s retina was better at predicting how they had scored on cognitive tests than tests revealing the density of brain plaques-clumps of beta-amyloid protein-present in the brain.īased on this new work-which was done using cadavers and tissues samples-several clinical trials are underway to determine if measuring amyloid deposits in the retina is an accurate way to diagnose early stage Alzheimer’s disease in living patients. Koronyo-Hamaoui’s team found that higher levels of the beta-amyloid protein-a hallmark of Alzheimer’s disease-in the retina corresponded to higher levels in the brain and more severe cognitive decline. Lerner, a neurologist with University Hospitals Cleveland Medical Center in Ohio who has treated patients with dementia for more than 30 years. Examining the eye may seem an unlikely strategy for Alzheimer’s screening, but in fact “it’s the only part of the central nervous system that you can see directly in a living person,, so people have been looking at the eye in Alzheimer’s disease for quite a while,” says Alan J. Located in the back of the eye, the retina translates light into electrical signals that travel to the brain. New drugs on the market, like lecanemab, for example, target patients with mild impairment before the symptoms become irreversible. If clinicians could reliably diagnose the disorder in this period before symptoms appear, they could try interventions to slow down its progression. “Alzheimer’s disease starts very early on in terms of the pathological changes, which can occur decades before symptoms do,” says Maya Koronyo-Hamaoui, a neuroscientist at Cedars Sinai Medical Center in Los Angeles who led the new study and collaborated with researchers in Italy and Australia. It is often said that eyes are windows to the soul, but according to recent research, they may also reveal early signs of Alzheimer’s disease, a neurodegenerative ailment that affects more than six million people in the United States and 55 million people worldwide.Ī seven-year analysis has connected physical changes in a region of the eye called the retina to what happens in the brain during Alzheimer’s, starting from its earliest stages when patients exhibit only mild cognitive impairment.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
